The conjunctiva is a very thin, transparent membrane (mucous membrane) that covers and protects the white part of the eye (called the sclera) and the inside of the eyelids. Its main functions are to protect and lubricate the rest of the external ocular structures against aggressive agents, and to provide immune defense. The most common aggressors belong to one of three groups: allergens, microorganisms and toxins.
Allergic conjunctivitis is an inflammation of the conjunctiva triggered by allergens. The most prominent symptoms of allergic conjunctivitis are: redness, itching and tearing. These symptoms are very bothersome and, if they are intense, will greatly affect activities of daily living and may interfere with sleep. Therefore, a correct diagnosis and appropriate treatment is very important, not only to improve the symptoms, but also to avoid aggravation and complications.
What is Allergic Conjunctivitis?
It is estimated that at least 20% of the population suffers from allergic conjunctivitis. Allergic conjunctivitis rarely appears in isolation. It is usually associated with other allergic conditions, especially allergic rhinitis – 70% to 80% of people who suffer from allergic conjunctivitis have allergic rhinitis, because the mucous membranes of the eyes and nose respond in the same way to airborne allergens (substances with characteristics that can trigger allergic reactions), and both react in the same way.
Symptoms such as nasal itching, discharge, nasal congestion and sneezing may be associated with this.
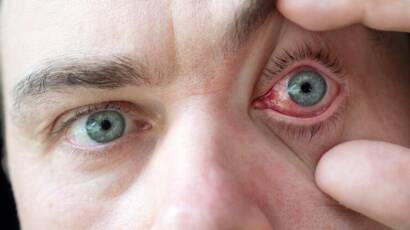

The eye conjunctiva and nasal mucosa have specific immune cells to respond to substances identified as foreign or irritating, leading to a strong inflammatory response, with the production of secretions (tears or nasal discharge) in an attempt to release, to eliminate the unwanted substance.
As with other allergies, the triggers of allergic conjunctivitis are innocuous for most people. However, when the immune system is overstimulated by substances that disrupt the system (certain types of food and food additives, airborne toxins, etc.), it reacts excessively, leading to intense inflammatory conditions.
The main triggers of allergic conjunctivitis are: pollens; dust mites; animal dander; molds and mildews; detergent, flavoring and bleach vapors; gases and dust from atmospheric pollution; among others.


Conjunctivitis can also be caused by infectious agents – infectious conjunctivitis – and toxic agents (in the workplace, chemical accidents) – toxic conjunctivitis. These two types of conjunctivitis can be more serious if they are not diagnosed early and treated effectively.
Symptoms of Allergic Conjunctivitis
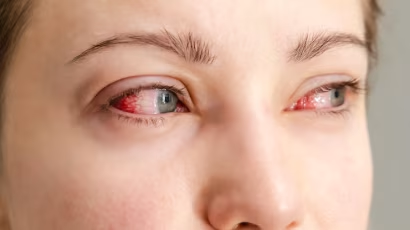
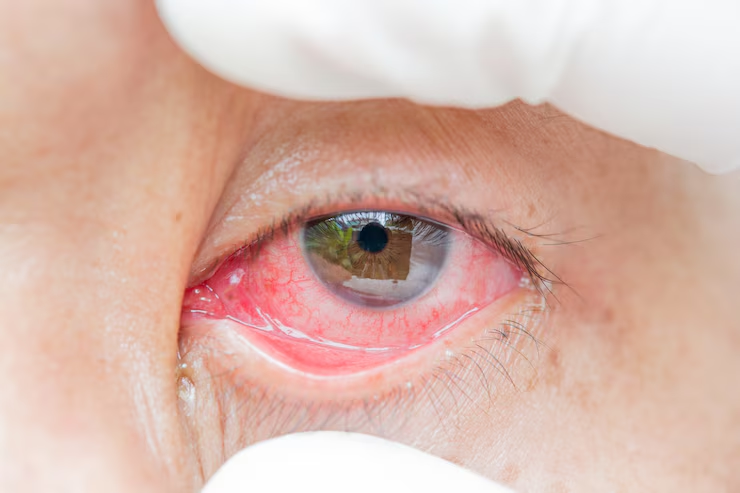
The symptoms of allergic conjunctivitis, which can vary in intensity, are: red eyes, burning eyes with intense itching, profuse tearing, edema (swelling) of the eyelids, edema of the conjunctiva, a feeling of “sand” in the eyes, and “thickening” (slight papillary hypertrophy) of the palpebral conjunctiva.
The symptoms usually affect both eyes equally and may not all be present at the same time. These symptoms can be annoying to the eye, but in general they don’t cloud vision unless they become very intense. There may be photophobia (intolerance to light) in more exuberant cases.
Allergic conjunctivitis, like allergic rhinitis, can be seasonal, related to pollination, so it appears in spring and early summer, and autumn; or in other seasons, depending on the local terrain and flora. If it continues throughout the year or for longer periods, it is called persistent or perennial, because it remains.


Diagnosis of Allergic Conjunctivitis
Although allergic conjunctivitis can be very disruptive to life and well-being, not least because it can last for prolonged periods, toxic conjunctivitis requires immediate and safe treatment, and infectious conjunctivitis requires timely, correct diagnosis and effective, specific treatment
The clinical diagnosis should be made by a doctor, but may require observation by a specialist ophthalmologist or allergist to ensure a more reliable and specific diagnosis.
The diagnosis of allergic conjunctivitis is based on observation and, essentially, on clinical history and the presence of other concomitant allergic disorders, such as rhinitis and allergic asthma. It may be necessary to carry out blood tests to identify specific antibodies, and skin prick tests with allergens (“allergy tests”) in persistent or difficult-to-control cases, to identify the possible allergens responsible.
Infectious conjunctivitis is caused by viruses (in most cases) or bacteria. In these cases, conjunctivitis may only affect one eye, but if left untreated, it can infect the other. Although some of the symptoms of allergic conjunctivitis can be common to those of infectious conjunctivitis, such as red eyes, tearing, a feeling of “sand” in the eyes, there are differences between the two. In allergic conjunctivitis there is a history of allergy and the itching is usually much more intense, as is the tearing and swelling of the eyelids. In infectious conjunctivitis, the eye secretions are purulent (yellowish or greenish) and sticky, and the itching is less or non-existent.
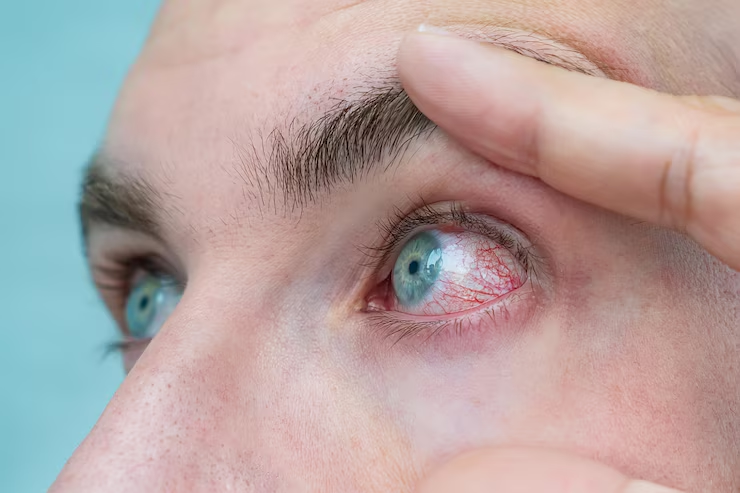

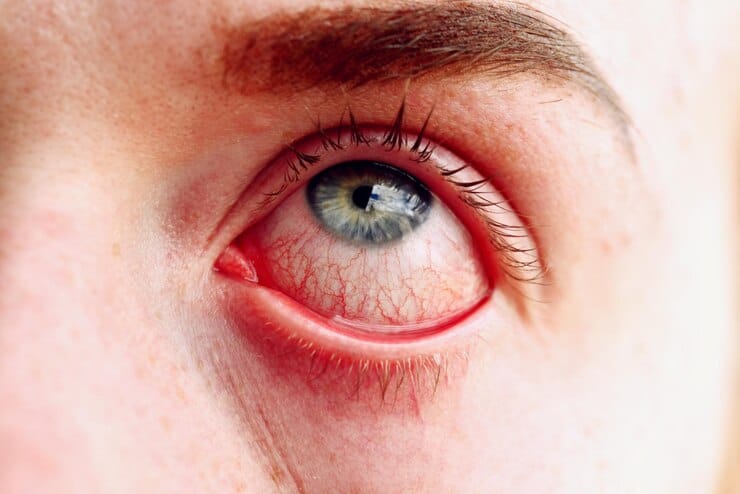
Toxic conjunctivitis, caused by direct contact with a toxic substance (splashing or accidental spillage of a chemical, industrial fumes, altered cosmetics, for example), requires specialized, safe and rapid intervention. These situations can become serious if left untreated. However, in the majority of cases, it is due to intolerance to the prolonged use of some of the components of medicines used to treat long-term eye conditions, such as eye drops or topical antibiotics and topical anesthetics (topical – directly applied to the eye).
Ocular allergic reactions can have multiple origins and the mechanisms of reactivity in each person can be diverse and individual. Therefore, not all eye allergies correspond to allergic conjunctivitis, although they may have some common symptoms.
How Long Does Allergic Conjunctivitis Last?
How long does allergic conjunctivitis last?
There is no single response. Its duration varies depending on the type of allergens and how long they remain in the affected person’s environment, as well as the presence of other concomitant allergic conditions such as asthma and allergic rhinitis. If it is seasonal allergic conjunctivitis, it can last throughout the entire pollination season if preventative measures and appropriate treatment are not taken. Thus, it can last from just a few days to around two weeks, or persist for weeks or months in chronic situations, where allergens remain in the environment (namely: dust mites, animal dander and occupational exposure), and there can be oscillation with periods of worsening and relief of symptoms.
A specialist doctor should be consulted, except in the case of mild, short-lived symptoms and without purulent secretions; and specialist medical assessment should be carried out quickly in the case of alarm symptoms: eye pain, photophobia (intolerance to light), reduced or blurred vision, very marked redness, use of contact lenses.
Treatments for Allergic Conjunctivitis
Treatment should be conducted according to the severity of the symptoms, with the aim of stopping or attenuating the inflammatory cascade associated with the allergic response, with consequent relief of symptoms and prevention of complications associated with chronic inflammation. The treatment of allergic conjunctivitis includes four areas of intervention: preventive strategies (to reduce exposure to the allergen/s), non-pharmacological measures, pharmacological treatment and immunotherapy.
Non-pharmacological measures include:
- wearing sunglasses to minimize contact with airborne allergens and improve photophobia;
- applying cold compresses can also be useful for relieving itching, reducing redness and swelling of the eyelids;
- the use of ocular lubricants (artificial tears or saline solution) can reinforce the barrier function of the ocular surface and good eyelid hygiene by removing allergens and inflammatory cells.
In general, these measures are not enough to resolve the symptoms, but they can help to reduce them.
Pharmacological measures:
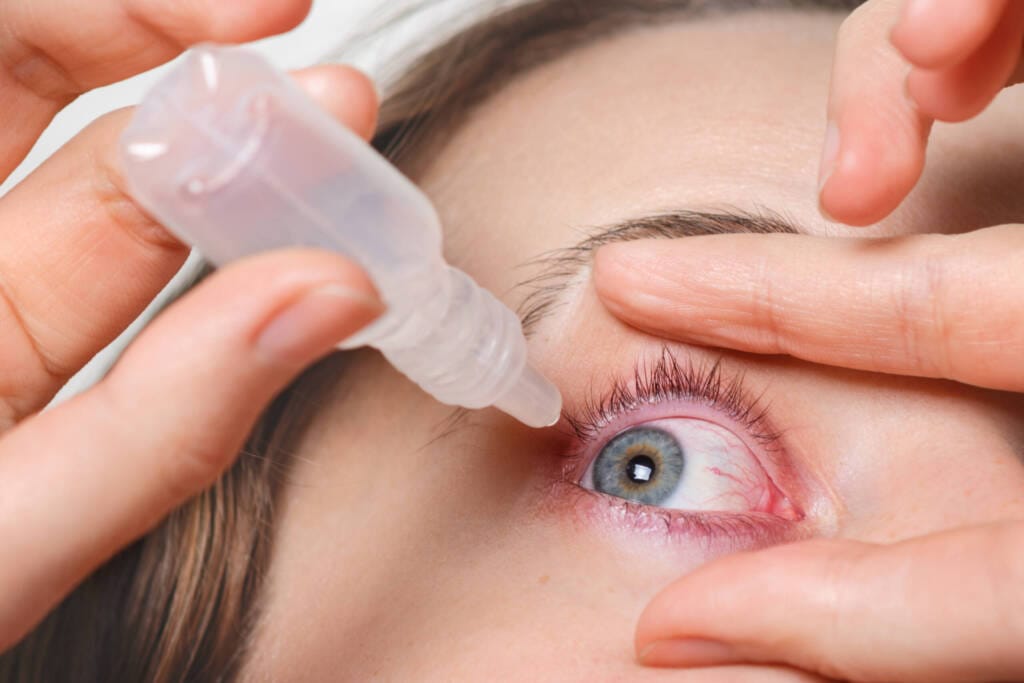
Pharmacological measures use drugs that are applied directly to the eyes (topical use), such as eye drops or ointments. This is the preferred approach due to its good efficacy and low systemic effects (acting on the whole body). When treating allergic conjunctivitis associated with allergic rhinitis or asthma, oral systemic medication may be recommended.
The main categories of drugs used are:
- those that slow down the allergic reaction cascade (antihistamines and mast cell stabilizers),
- those that reduce redness and edema (vasoconstrictors),
- those that counteract inflammatory symptoms (non-steroidal anti-inflammatory drugs and corticosteroids), but which must be used with great care.
Immunotherapy with allergens (by skin prick or sublingual application) remains the only therapeutic option capable of modifying the natural history of allergic disease, but requires specific clinical criteria. It is recommended when moderate to severe symptoms persist and interfere with the patient’s quality of life, despite ongoing optimized treatment.

Prevention of Allergic Conjunctivitis
The patient should be explained the allergen avoidance measures (avoidance, minimization and withdrawal) aimed at the allergens previously identified in the diagnostic study. These measures also apply to other allergic diseases such as allergic rhinitis.
These include: scheduling outings during the pollination season; wearing sunglasses; measures to sanitize the house and indoor air, and keeping animals away in cases of allergy to dust mites and animal dander;
In the workplace: removal or protective measures against allergens; and also, whenever possible, the use of certified air purification equipment (HEPA) to remove all allergenic particles suspended in indoor air. This last measure can help to drastically reduce symptoms, since most people spend the majority of their daily time indoors (meals, sleeping, leisure, and working from home).
Conclusion
There are a multitude and complexity of other eye allergies, apart from allergic conjunctivitis, which go beyond the scope of this article, some of which are potentially serious if they are not correctly diagnosed and treated, so an assessment by an ophthalmologist is advisable in the event of persistent symptoms. Medical assessment is extremely important in cases of non-seasonal ocular allergies, and seasonal allergies that worsen significantly, as there are clinical conditions that can rapidly evolve into very serious situations (see “alarm symptoms” above) that require timely medical intervention.
For the prevention of symptoms and long-term eye health, all measures that reduce contact with allergens, which are mostly found inside the home, are useful: keeping it clean and sanitized (frequent washing of bed linen, curtains, cushions); reducing or eliminating surfaces that accumulate dust and allergens (carpets, rugs, fabric-covered sofas); eliminating or reducing contact with animals, especially in the bedroom; and, where possible, purifying indoor air with HEPA equipment.
Bibliography
- Mota D, Vasconcelos MJ, Moreira A, Delgado L, Palmares J, Silva D. Alergia ocular: Da abordagem clínica ao tratamento. Rev Port Imunoalergologia 2024; 32 (1): 9-27. https://www.spaic.pt/client_files/rpia_artigos/artigo-de-reviso(17).pdf
- Marback PMF, Freitas D, Paranhos Junior A, Belfort Júnior R. Aspectos clínicos e epidemiológicos da conjuntivite alérgica em serviço de referência. Arq. Bras. Oftalmol. 70 (2) • Mar 2007. DOI: 10.1590/S0004-27492007000200022
- Leonardi A, Piliego F, Castegnaro A, Lazzarini D, Valerio L, Mattana P, et al. Allergic conjunctivitis: A cross-sectional study. Clin Exp Allergy. 2015;45(6):1118-25. DOI: 10.1111/cea.12536.
- Palmares J, Delgado L, Cidade M, Quadrado MJ, Filipe HP. Allergic conjunctivitis: A national cross-sectional study of clinical characteristics and quality of life. Eur J Ophthalmol. 2010;20(2):257-64. DOI: 10.1177%2F112067211002000201.




